Despite an overall shift toward value-based care, payment and financing models in the United States remain largely tied to clinical services and have not incorporated services linked to the social determinants of health, stunting reform that could make the benefits of community-wide population health a reality.
AcademyHealth’s Payment Reform for Population Health (P4PH) initiative, funded by the Robert Wood Johnson Foundation, works to identify the challenges associated with linking the health care payment system to geographically-based population health. Interviews with key stakeholders, site visits, and internal collaboration have pushed to the surface a number of barriers that stand in the way. As the initiative approaches its halfway mark, AcademyHealth has begun supporting activities to address these barriers and identify the community stakeholders that enable population health-focused payment models to thrive.
Through cross-team collaboration and co-creation, AcademyHealth has developed a robust project framework (see Image 1 below) to guide further investigations into the financing/reimbursement mechanisms used by health plans and providers to support non-clinical population health-related social support services. Employing an Emergent Strategy approach, this visual framework continually evolves as new findings – particularly those related to barriers – emerge.
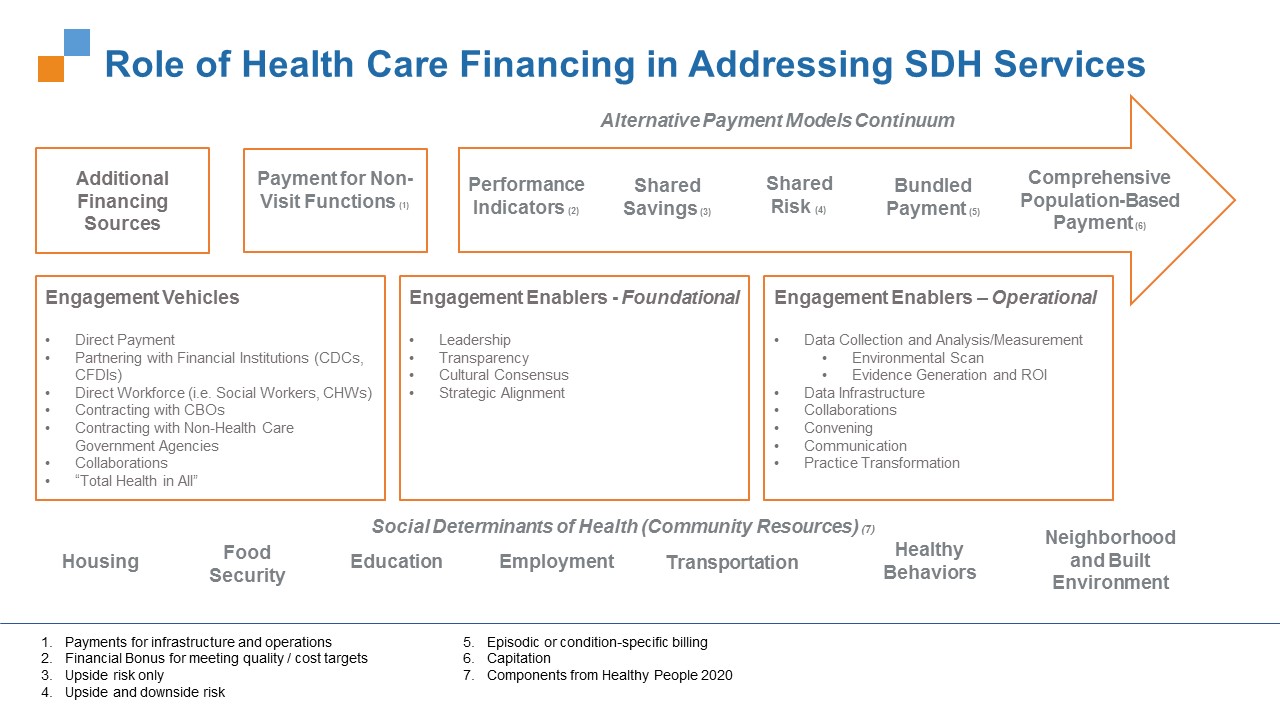
The framework illustrates how financing sources, including alternative payment models (APMs) and other funding sources can pay for population health-based services focused on the social determinants of health (i.e., housing, food security, education, employment, transportation, healthy behaviors, and neighborhood and build environment).
The array of funding sources is arranged from left to right in the top arrow of the framework and are categorized by Additional Financing Sources (e.g., community benefit funds, grants, reserves, etc.), Payment for Non-Visit Functions (i.e., payments for infrastructure and operations), and APMs. The APMs are arranged on a continuum from the least comprehensive, more traditional APMs – such as Pay for Performance – to the most comprehensive “population-based payments” – such as global payments.
Research, interviews with key stakeholders, and site visits helped inform the P4PH on how payments flow can through “Engagement Vehicles and Enablers” to effectively support the social determinants of health, as illustrated in the middle portion of the framework. An Engagement Vehicle describes where health care systems directly fund services and/or non-health care providers and organizations (including community-based organizations and public health agencies) that focus on addressing the social determinants of health. An Engagement Enabler describes where the health care system can more broadly support activities and infrastructure to link clinical and community-based services. Enablers can be either “Foundational” (e.g., providing leadership or the need for cultural consensus) or “Operational” (e.g., data infrastructure or on-the-ground convenings). Understanding the details of Enablers and Vehicles can help more clearly identify strategies that have a significant capacity to overcome the most pressing barriers to improving population health.
As the P4PH team moves steadily into Phase Two – “Catalyzing Action” – the framework plays a critical role in mapping and testing the potential barrier-busting activities that will be supported by the initiative. Barriers that have risen to the top during Phase One can be classified into the following topic areas:
- Payment Models and Financing
- The Role of a Neutral Convener
- Cross-sector Collaboration
- Data Infrastructure/ Population Metrics
- Business Case / Return-On-Investment / Evidence Base
Despite the complex nonlinear nature of the issue, AcademyHealth’s range of expertise and diverse membership has positioned the P4PH team to capture significant findings. Using the aforementioned framework as a guide, AcademyHealth will strive to identify the most common barriers health systems experience in supporting upstream investments, align with a variety of collaborators, and strategically develop activities to help health systems realize lasting, meaningful change.
Stay tuned here, at the AcademyHealth blog, for updates on our initiative’s progress and emerging findings. If you are doing related work, please contact Enrique Martinez-Vidal; we’d like to include you in our efforts!